This article was co-authored by Sarah Tewhey, L.Ac., acupuncturist, herbalist and doula
Breech (feet first) position in the latter part of the third trimester of pregnancy is uncommon, but can prevent the possibility of a vaginal birth. In the United States, standard of care in breech term pregnancy is planned cesarean section, with over 90% of breech babies at term in 2019 being born via cesarean birth (1). While only 3-4% of pregnancies are breech at term (2), this small percentage represents thousands of cesarean births each year. Planned cesarean birth due to malposition carries risk, can significantly affect the pregnant person if they had hopes for a vaginal birth, impacts maternal outcomes including postpartum recovery and adds costs to the healthcare system as a whole. It is to the benefit of both pregnant people and hospitals to have a range of corrective options to help babies turn cephalic (head down) prior to planning a cesarean birth.
Why Do We Need to Explore Other Ways of Correcting Breech Presentation?
The most common intervention for breech presentation is External Cephalic Version (ECV). During an ECV, a trained healthcare provider uses their hands on the outside of the abdomen to manually turn the baby into a cephalic position. ECV is typically attempted at 36-37 weeks gestation and is 50%-60% effective (1). However, ECV is not routinely offered to all pregnant people whose babies are breech, may not be accessible in some locations where a trained provider is not available and carries some risk of complications. In addition, ECV can be physically painful and create emotional stress. For these reasons ECV is not an intervention that all pregnant people are offered or choose to attempt.
Moxibustion and acupuncture provide potential as an additional intervention for correcting a breech presentation that is cost effective and low risk (3). For parents, learning that their baby is breech can create a range of complex emotions. Parents may face both internal and external pressures when making decisions around potential interventions (6). Choice and shared decision making are important to pregnant people. Providing an option for moxibustion and acupuncture may be a welcome addition to the conversation between parents and their prenatal providers when making decisions around interventions for breech. In clinical practice it is increasingly common for midwives and physicians to refer pregnant people to acupuncturists prior to trying other interventions such as an ECV.
How Might Acupuncture and/or Moxibustion (Moxa) be Used?
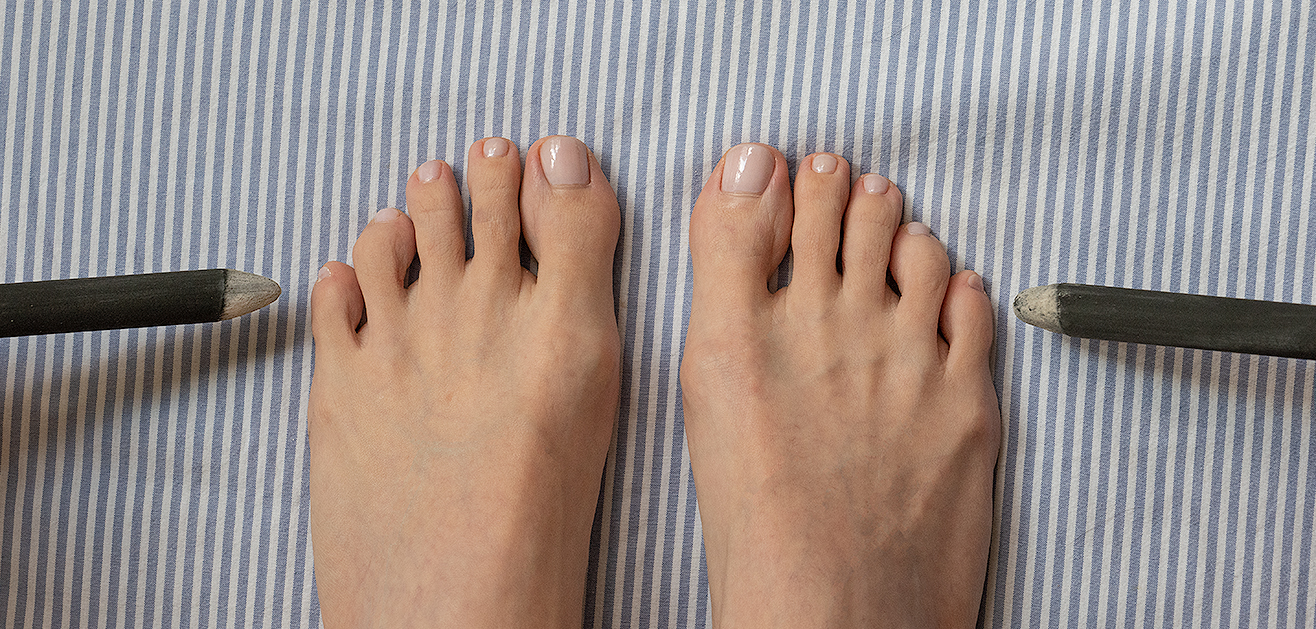
Acupuncture and moxibustion have been used for centuries in East Asian Medicine for a wide array of concerns. Acupuncture is the insertion of fine needles into specific points on the body for the purpose of influencing a myriad of physical and mental/emotional conditions. Moxibustion is the application of heat to acupuncture points by burning preparations of the herb Ai Ye or Artemisia argyi near the skin. For the purpose of correcting fetal position, moxa is generally used in the form of a rolled cigar-like stick to indirectly warm a point located on the outer edge of the 5th toe known as Zhi Yin or Urinary Bladder 67. The moxa stick is moved in a slow pecking motion to gently warm the point once or twice daily for 15-30 minutes each session.
While more research into the most effective dosage and timing to correct malpresentation is needed, there are current practices within the acupuncture community which are regarded as the standard of care. In a 2013 Delphi survey (5) of 12 acupuncturists selected due to their expertise in providing care during pregnancy, 80% of respondents indicated that treatment should commence between 34-35 weeks. 90% agreed that home use of moxibustion with smokeless moxa sticks was the most appropriate method and 70% indicated treatment for a minimum of 10 days for at least 30 minutes a day to be optimal. All respondents agreed Urinary Bladder 67 is the preferred point for administering the moxibustion. 50% of respondents indicated that treatment with acupuncture was also an important part of care in correcting malpresentation. All respondents felt that moxibustion could safely be administered at home after instructions on use and safety were provided by an acupuncturist.
After receiving education on use, pregnant people can then self-administer the moxibustion outside a clinical setting. Moxibustion as an optional intervention can provide pregnant people with increased choice and assist them in feeling more in control of an unexpected and often stressful situation. Daily treatment at home may also create feelings of relaxation and increased connection with their partner, who can be involved with administering the treatment (6). All of these factors can positively impact a pregnant person’s perception of their pregnancy and birth. After being seen for acupuncture and performing home treatment, babies may be cephalic at their next primary care prenatal visit. If the treatment is ineffective, ECV is still an option at 36-37 weeks gestation.
In addition to acupuncture and moxibustion, some pregnant people may also receive guidance on positional exercises, chiropractic and/or pelvic physical therapy to help encourage their baby to turn. All of these methods can work in tandem alongside acupuncture and moxibustion and usual care.
What does the Research Show?
This plain-language summary will primarily focus on the results of a type of study called a Systematic Review (SR). SR’s combine the results of several individual studies that are somewhat similar. For this reason, SR’s are more important and impactful than looking at one or two studies alone.
A 2012 Cochrane Systematic Review by Coyle et al. (7) looked at 8 trials (1346 participants) that assessed the use of moxibustion, acupuncture, postural techniques and usual care for breech presentation. Of those 8 trials, 3 studies (594 participants) compared moxibustion treatment alone to usual care and found no significant difference in the rate of cephalic babies at birth. However, a more recent 2021 Systematic Review by Liao et al. (8) looked at the same 3 studies plus an additional 10 trials (2063 participants) and found that those using moxibustion at UB 67 versus those receiving usual care did have an increased rate of cephalic presentation at birth.
These two SR’s (7,8) also analyzed trials using moxibustion combined with another type of treatment such as acupuncture or postural techniques. A few studies even looked at acupuncture alone (without moxibustion). Both SR’s found that acupuncture plus moxibustion resulted in a higher number of head-down babies at birth compared with usual care. Only the 2012 Cochrane Review looked at moxibustion used alongside postural techniques versus postural techniques alone. It found that across those 3 studies, there was an increase in the number of head-down babies at birth in those using moxibustion.
Finally, the 2021 Systematic review (8) looked at trials which compared acupuncture alone to a control group. Two studies (146 participants) found no difference in the number of head-down babies at birth. Because this finding is represented by only two studies and both were small, additional, larger studies are needed to have more certainty about the impact of acupuncture alone on babies’ position.
Does It Really Matter Which Acupuncture Point Gets Moxibustion?
Vas et al. (9) conducted a study in 2013 which tried to determine if the UB 67 acu-point (at the outer edge of the 5th toenail) is specifically helpful with turning breech babies. This trial was large and well-designed with three groups: those who had moxibustion at the usual point UB 67, those who had moxibustion at an “inactive” point on the inner edge of the 1st toenail and those who had usual care. The study found that moxibustion on UB 67 resulted in head-down babies in 58% of participants, while the other two groups had significantly fewer head-down babies (43% and 45%). Although additional studies are needed before making definitive conclusions, because this study was quite large (406 participants) and well designed it indicates that there may be something unique about the UB 67 acu-point that is helpful for fetal malpresentation.
Moxibustion Included in Clinical Guidelines
Moxibustion and acupuncture are included in the (UK) 2017 Royal College of Obstetricians and Gynecologists (RCOG) Green-top Guidelines for ECV and Reducing the Incidence of Term Breech Presentation (10). This document represents the first time that these methods of treatment have been included as a clinical guideline by a major professional organization within the field of Obstetrics. The guidelines cite both the 2012 Cochrane Review and the 2013 Vas et al. study and recommend that pregnant people may wish to consider the use of moxibustion at 33-35 weeks gestation. The recommendation also cites that acupuncture combined with moxibustion may further reduce the number of cesarean sections and emphasizes the importance of choosing a trained practitioner when seeking out this type of treatment.
Risk Factors and Contraindications
There are some instances where acupuncture and moxibustion may present increased risk or be contraindicated when assisting babies to turn. These are similar to contraindications for ECV and may include Olgiohydraminos (too little amniotic fluid); Polyhydramnios (too much amniotic fluid); a history of vaginal bleeding in pregnancy, known fetal abnormalities or growth issues, history of PROM or premature labor, gestational diabetes, hypertension; placenta previa; bicornuate uterus; twins or other non-singleton pregnancy and any concern in which ECV is contraindicated by the primary care provider. In these situations the decision on whether to use moxibustion should be made via collaboration and mutual agreement between the pregnant person, the acupuncturist and the primary prenatal care provider.
Finding a Trained Practitioner
Most acupuncturists receive some limited training in perinatal care, however working in this specialty safely and effectively requires additional post-graduate education. When choosing an acupuncturist, ask questions about what education and experience they have in treating pregnant people. Local midwives, doulas, Labor and Delivery nurses and physicians will be familiar with acupuncturists who specialize in perinatal health and who are qualified to help. These types of providers can make referrals to well trained practitioners.
Additionally, in choosing an acupuncturist, make sure they are aware of the methods, safety concerns and contraindications to using moxibustion for breech. Practitioners should also provide thorough instructions and support to the pregnant person for home moxibustion use.
Resource Links
Maternity Acupuncture Mentoring and Peer Support (MAMPS) provides high quality post-graduate education and support to acupuncturists who wish to provide care in pregnancy, birth and postpartum. Visit https://www.mamps.org/ for further information on postgraduate training as well as practitioner safety guidelines for the treatment of breech presentation.
The Obstetrical Acupuncture Association (OBAA) provides a resource for both pregnant people and their care providers to find acupuncturists in their area who demonstrate an elevated standard of care and safety within the field of perinatal care. They can be found at https://ob-acupuncture.com/
Spinning Babies: a resource on various modalities and postural exercises for turning malpositioned babies
The Miles Circuit: a set of postural exercises for rotating the baby into an ideal position for birth
Sources
- Dekker, Rebecca. “Evidence On: Breech Version.” Evidence Based Birth®, 29 Mar. 2021, evidencebasedbirth.com/what-is-the-evidence-for-using-an-external-cephalic-version-to-turn-a-breech-baby/
- Hofmeyr GJ, Kulier R, West HM. External cephalic version for breech presentation at term. Cochrane Database of Systematic Reviews 2015, Issue 4. Art. No.: CD000083. DOI: 10.1002/14651858.CD000083.pub3. Accessed 22 May 2022.
- I. van den Berg, G. Kaandorp, J. Bosch, J. Duvekot, L. Arends, M. Hunink, Cost-effectiveness of Breech Version by Acumoxa for women with a breech fetus at 33 weeks gestation: A modeling approach, European Journal of Integrative Medicine, Volume 1, Issue 4, 2009, Page 257, ISSN 1876-3820, https://doi.org/10.1016/j.eujim.2009.08.068
- Morris, Sara, et al. “Women’s Experiences of Breech Birth Decision Making: An Integrated Review.” European Journal of Midwifery, vol. 6, no. January, 25 Jan. 2022, pp. 1–14, 10.18332/ejm/143875.
- Smith CA, Betts D. The practice of acupuncture and moxibustion to promote cephalic version for women with a breech presentation: implications for clinical practice and research. Complement Ther Med. 2014 Feb;22(1):75-80. doi: 10.1016/j.ctim.2013.12.005. Epub 2013 Dec 12. PMID: 24559820.
- Mitchell M, Allen K. An exploratory study of women's experiences and key stakeholders views of moxibustion for cephalic version in breech presentation. Complement Ther Clin Pract. 2008 Nov;14(4):264-72. doi: 10.1016/j.ctcp.2008.05.002. Epub 2008 Jul 22. PMID: 18940713.
- Coyle ME, Smith CA, Peat B. Cephalic version by moxibustion for breech presentation. Cochrane Database of Systematic Reviews 2012, Issue 5. Art. No.: CD003928. DOI: 10.1002/14651858.CD003928.pub3
- Liao JA, Shao SC, Chang CT, Chai PY, Owang KL, Huang TH, Yang CH, Lee TJ, Chen YC. Correction of Breech Presentation with Moxibustion and Acupuncture: A Systematic Review and Meta-Analysis. Healthcare (Basel). 2021 May 22;9(6):619. doi: 10.3390/healthcare9060619. PMID: 34067379; PMCID: PMC8224784.
- Vas J, Aranda-Regules JM, Modesto M, Ramos-Monserrat M, Barón M, Aguilar I, Benítez-Parejo N, Ramírez-Carmona C, Rivas-Ruiz F. Using moxibustion in primary healthcare to correct non-vertex presentation: a multicentre randomised controlled trial. Acupunct Med. 2013 Mar;31(1):31-8. doi: 10.1136/acupmed-2012-010261. Epub 2012 Dec 18. PMID: 23249535.
- Impey LWM, Murphy DJ, Griffiths M, Penna LK on behalf of the Royal College of Obstetricians and Gynaecologists. External Cephalic Version and Reducing the Incidence of Term Breech Presentation. BJOG 2017; 124:e178–e192.
- Cardini F, Weixin H. Moxibustion for correction of breech presentation: a randomized controlled trial. JAMA. 1998 Nov 11;280(18):1580-4. doi: 10.1001/jama.280.18.1580. PMID: 9820259.
- Cardini F, Lombardo P, Regalia AL, Regaldo G, Zanini A, Negri MG, Panepuccia L, Todros T. A randomised controlled trial of moxibustion for breech presentation. BJOG. 2005 Jun;112(6):743-7. doi: 10.1111/j.1471-0528.2005.00634.x. PMID: 15924530.
- Guittier MJ, Pichon M, Dong H, Irion O, Boulvain M. Moxibustion for breech version: a randomized controlled trial. Obstet Gynecol. 2009 Nov;114(5):1034-1040. doi: 10.1097/AOG.0b013e3181bc707a. PMID: 20168104.
- Higashihara A, Horiuchi S. Smoke or smokeless moxibustion treatment for breech presentation: A three-arm pilot trial. Jpn J Nurs Sci. 2021 Oct;18(4):e12426. doi: 10.1111/jjns.12426. Epub 2021 May 17. PMID: 33999503; PMCID: PMC8518843
- Helene M. Langevin, Peter M. Wayne, Hugh MacPherson, Rosa Schnyer, Ryan M. Milley, Vitaly Napadow, Lixing Lao, Jongbae Park, Richard E. Harris, Misha Cohen, Karen J. Sherman, Aviad Haramati, Richard Hammerschlag, "Paradoxes in Acupuncture Research: Strategies for Moving Forward", Evidence-Based Complementary and Alternative Medicine, vol. 2011, Article ID 180805, 11 pages, 2011. https://doi.org/10.1155/2011/180805
- Hopper Koppelman.. Acupuncture: An Overview of Scientific Evidence. Evidence Based Acupuncture. 2018. https://www.evidencebasedacupuncture.org/acupuncture-scientific-evidence/